Abdominal aortic aneurysm treatment Perth
Abdominal aortic aneurysm: All your questions answered

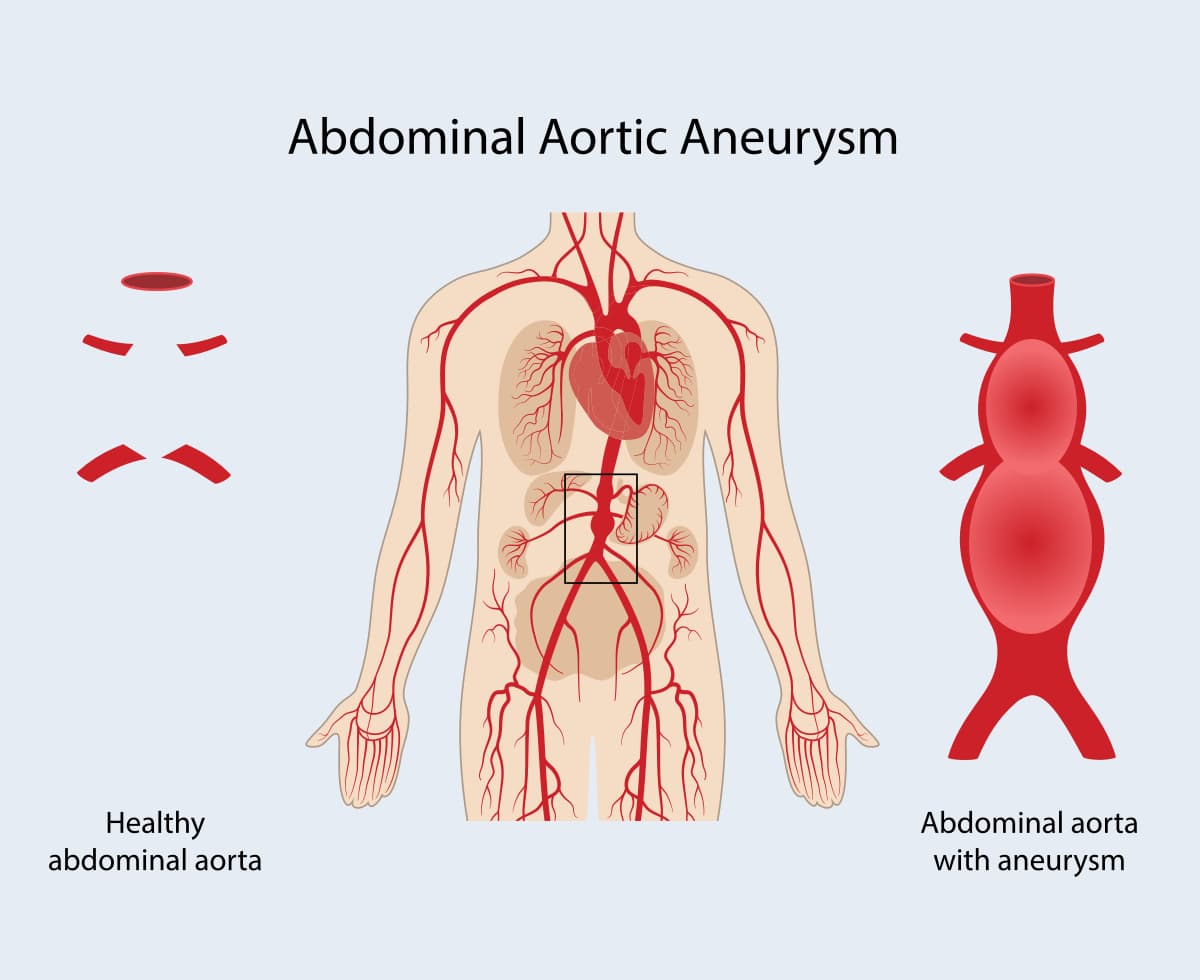
The aorta is the largest artery in the body and it transports the blood from the heart to the rest of the body. If you have an abdominal aortic aneurysm, it means that the wall of your aorta has weakened. Pressure from inside the aorta causes this weakened area to bulge. When the aneurysm remains under 5 cm in diameter, there’s not much reason for concern. But when it’s bigger than 5 cm, and it bursts, it can cause life-threatening bleeding.
How do I know if I have an abdominal aortic aneurysm?
If you are reading this article, chances are that you or a family member have looked into information about an abdominal aortic aneurysm (AAA) because symptoms were diagnosed. It was probably picked up by an ultrasound or CT scan, performed for another reason.
Most patients with an abdominal aortic aneurysm do not know that they have one and it gets picked up during a scan for other purposes.

Vascular Surgeon Perth
Adjunct Clinical Associate Professor at Curtin University
Before we dive into the treatment options for this condition, let’s explain first what it is and what can be the causes to suffer from an AAA.
What is an abdominal aortic aneurysm?
The aorta is the largest artery in your body and it transports oxygen-rich blood from your heart to the rest of your body. If the wall of the aorta weakens, pressure can cause this weakened area to bulge.
Aneurysms may develop at any site, but the most common sites remain in the abdomen. Most aneurysms slowly increase in size and the problem with aortic aneurysms is that when they get to a certain size, they may burst resulting in bleeding and possibly death. The treatment aims to try to decrease the growth rate and repair the aneurysm before the risk of bursting becomes high.
The risk of a small AAA bursting at a high altitude is very low. If the AAA is between 4-5 cm the risk is about 1% per year, and if it is 3-4 cm it is about 0.1% per year. Theoretically, changes in cabin pressure when flying can increase the risk of rupture. But in reality, that risk is not higher than at any other time.
6 risk factors you need to be aware of
The weakening of the aortic wall is often caused by atherosclerosis, a build-up of plaque, which is a deposit of fatty substances and cholesterol.

Vascular surgeon Perth
Age
As you get older, your risk of abdominal aortic aneurysms increases. However, most people don’t develop one simply because they are getting older.
Male sex
Being male increases your risk too. The occurrence in males is 4 to 5 times greater than that of females. So women can get one too, but the rate of developing an abdominal aortic aneurysm is lower.
Smoking
Smoking is one of the biggest factors in developing an abdominal aortic aneurysm. Nicotine weakens the vessel wall, allowing the aneurysm to get bigger.
Family history
First-degree family members of patients with a diagnosed abdominal aortic aneurysm are at higher lifetime risk (up to 20%) of developing one.
High cholesterol levels
Studies have reported that higher circulating levels of total cholesterol (TC), low-density lipoprotein (LDL) cholesterol and lower high-density lipoprotein (HDL) cholesterol may be associated with an increased risk of abdominal aortic aneurysm (AAA).
High blood pressure
Hypertension or high blood pressure increases your risk of developing atherosclerosis.

What treatments are available for aortic aneurysms?
The aim of any treatment is to prevent the aneurysm from bursting.
The aim of any treatment is to prevent the aneurysm from bursting.
The treatment that is best for you is based on multiple factors:
- Your age and overall medical health
- Extent of the disease – the information we obtain is based on a CT scan
- Your tolerance of specific medications, procedures, or therapies
- Your treatment preference
Once you have a diagnosed AAA, you will need to control or modify the risk factors that cause the aneurysm to grow. This includes:
- Stopping smoking
- Losing weight if overweight
- Taking medications to thin the blood,
- Control high blood pressure and reducing the fat in your blood (statins).
Generally, when an aneurysm is smaller than 5cm in diameter, you will be monitored regularly to see if your AAA grows.
We tend to operate if the aneurysm is larger than 5cm in diameter, or if it grows more than 0.5 cm in 6 months. If you start to develop symptoms, we may also perform surgery.

Vascular surgeon Perth
Medical management
The choice of medical treatment depends on the presentation and your co-morbidities. You are likely to start on a blood thinner, something to control your cholesterol and blood pressure. Other risk factors that would also be managed include stopping your smoking habits, losing weight and exercising.
Open aortic aneurysm repair
In an open repair, an incision is made in the abdomen to repair the aortic aneurysm. In this procedure, the diseased artery is replaced by an artificial tube. This allows the blood to flow into the rest of the body, thereby preventing the bursting of the artery.
Most patients stay in ICU for 1 or 2 days and may leave the hospital in 7 days.
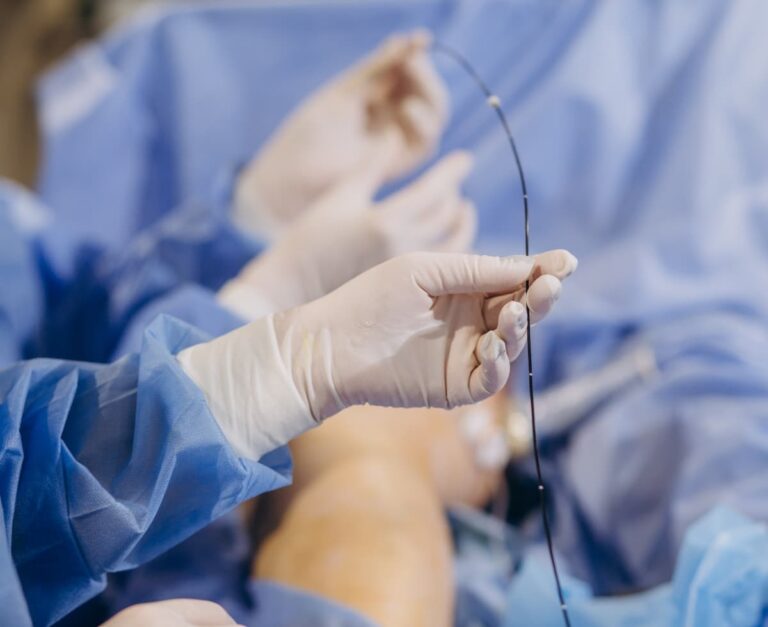
Endovascular aortic aneurysm repair (EVAR)
Endovascular stenting is a minimally invasive operation that allows the placement of stents in the aorta across the aneurysm. The stent allows the blood to travel in the stent rather than the aneurysm, preventing it from bursting. The stents are delivered via small incisions in your groin.
Most patients stay in ICU for 1 day and in the hospital for 2 to 3 days. After the operation, you will need a regular check-up with an ultrasound.
As a minimally invasive procedure, EVAR is gentler on your body. Benefits include
- Fewer days in the hospital
- Less discomfort during recovery
- Quicker return to daily activities
- Reduced risk of having a heart attack or dying around the time of your procedure than you’d have in open surgery
- Shorter procedure time than open surgery
Endovascular aneurysm repair is a safe procedure with a high success rate. But there’s always a chance of complications. These include
- Blood clots
- Endoleak – this occurs when blood fills the aneurysm sac after the procedure. The majority of endoleaks are safe – but certain types of endoleaks may need further procedures to close them
- Infection
- Kidney failure
- Bleeding
- Heart attack
Frequently asked questions
It generally takes days to weeks to get back to normal. Expect to stay in the hospital for 1-2 days and walk the day after the procedure. Most people return to work within a few weeks. Avoid lifting anything heavy for four to six weeks after your procedure.

About
Dr Altaf
As a vascular surgeon, I believe there is no one size fits all. This means appointments take as long until you fully understand the condition and are happy with my approach to get you the best treatment option.